< Back to Sanius content
Healthcare Industry Spotlight: Orlando Agrippa, CEO of Sanius Health “Revolutionising Patient Care: A Patient-Centred Approach to Flow and Discharge”
Sanius Health: On taking a patient-centred and clinically led approach to the issues around patient flow and discharge instead of the conventional operational flow approaches.
Empowering patients to understand better and manage their health
Sanius Health offers patients a unique, longitudinal view of their daily health outcomes. This means patients can access continuous digital engagement and remote monitoring, allowing for proactive health management outside secondary care settings.
“We focus on the patient’s individual requirements and have built Sanius Health around meeting unmet needs. Because of this, members of our community are seeing better outcomes, and systems experiencing less impact on flow.”
The importance of clinical engagement has allowed Sanius Health to accelerate adoption; the technology allows clinicians to view key information and use it to proactively manage care and support patients to adhere to their treatment plans, ultimately keeping them healthy and out of the hospital.
The advanced insights provided by Sanius Health can help identify and highlight potential health events that may occur outside of care settings. By catching these issues early, patients can receive prompt care and avoid hospital admissions, reducing the demand for emergency departments and the first entry point for healthcare.

Although SCD is one of the most common genetic conditions affecting people in England, it is consistently misunderstood and patients regularly do not receive the care they need. Medical staff are insufficiently educated on the condition, which has a significant negative impact on patient outcomes and can make patients reluctant to seek care, even in the case of an emergency.
Almost every single person with SCD has experienced their pain being ignored, dismissed or minimised by medical professionals. Racism is interwoven through their clinical encounters, with a concerningly high number of patients accused of being ‘drug seekers’ by A&E staff. Adam E., a member of Sanius Health’s ecosystem, is one of many who have opted to treat themselves at home rather going to hospital altogether due to discrimination:
‘Because of my condition, I need emergency opioids for pain relief. But because SCD is so rare, and not many A&E staff know or recognise what it is, this means that many assume that I’m just seeking drugs – not care.’
Socioeconomic Determinants of Health
Socioeconomic status contributes to poorer health outcomes in numerous ways, from obvious factors like access to high-quality specialist healthcare to more subtle – but no less impactful – things like housing, nutrition, air pollution levels in less affluent areas, sleep deprivation due to long unsociable working hours, and how much time they have available to dedicate to healthy habits. All of these factors stack the odds against people from lower socioeconomic backgrounds, and that is before SCD is added into the mix.
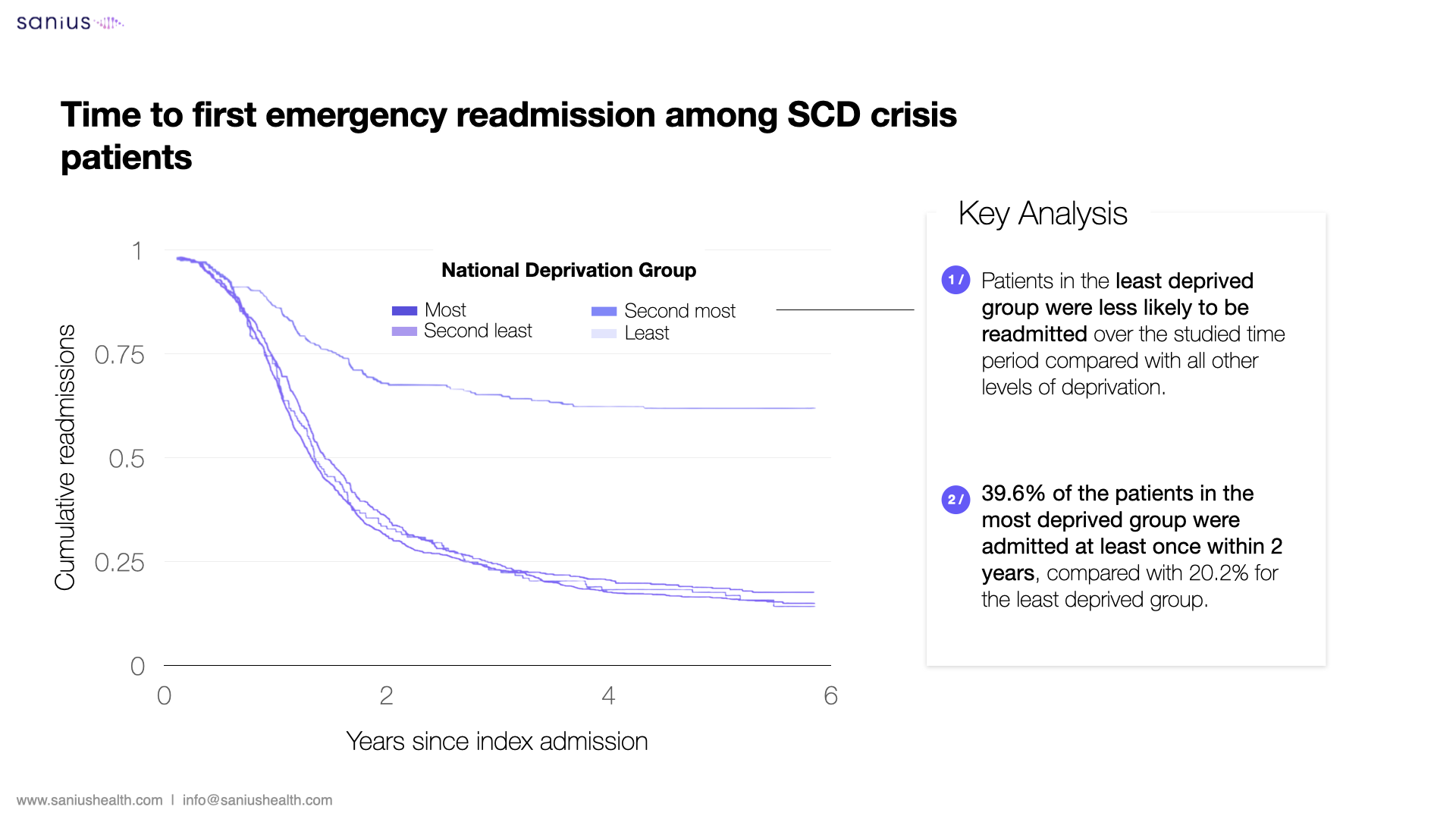
SCD patients from the most socio-economically deprived areas and with co-morbidities are at highest risk of both SCD readmissions and in-hospital mortality, and with 50% of patients most commonly treated for SCD living within the 50 most deprived areas of the country, this is a stark and urgent issue. Within London, for example, around 80% of all SCD admissions are from people living in the most deprived areas. Due to the financial ramifications of being in hospital – such as loss of pay, additional childcare costs, and potential job loss – people on low income may discharge themselves prematurely, putting their health further at risk.
People from lower socioeconomic backgrounds tend to have limited access to healthcare resources, whether that is the knowledge and tools necessary to manage their condition at home or access to specialists. Siobhan, a patient who is treated in one of the biggest specialist centres in the country, compares her experience to others who are less able to access the care they need:
‘I have a great team, and I am lucky that I am relatively close to the nearest specialist. However, a lot of people in the community are not so lucky. Because of their circumstances, many have to wait hours to receive care. Some aren’t able to at all, and access is difficult overall.”
Painful vaso-occlusive crises caused by SCD can be brought on by changes in temperature, dehydration, malnutrition, overexertion and stress – all of which are closely tied to socioeconomic factors and especially prevalent amidst the current cost of living crisis.
While the unpredictability of SCD can significantly impact people’s ability to work and study, it is both difficult and extremely stressful to claim government support in the form of PIP (Personal Independence Payment). 2019 government figures showed that only 1,350 people with SCD were receiving PIP payments – less than 10% of the estimated 15,000 people living with the condition in the UK. A lack of education and awareness about SCD among decision-makers throughout the PIP claim process continues to perpetuate this problem.
Health Literacy and Patient Empowerment
Promoting patient empowerment and self-management is our core focus at Sanius Health. Our tools help patients manage their wellbeing at home, predict crises before they happen so that users can take preventative measures, and have significantly reduced hospitalisations among our users. Identifying early signs of deterioration also helps patients identify when it is time to seek help, as well as alleviating some of the mental burden of determining when symptoms are ‘bad enough’ to do so.
When certain health metrics tip beyond a certain threshold, the Sanius Health app advises the user to seek urgent help; users have commented that this not only encourages them to act promptly but also validates their experience and effectively gives them ‘permission’ to seek the help they need.
Advances in Research and TreatmentSanius Health Advocating for Change and System Resilience Ahead of Winter 2023.
When trying to improve the lives of people with SCD we must look beyond the obvious medical aspects and tackle the wider inequalities that contribute to poorer outcomes for those in the community.
Empowering patients to play an active role in their care is crucial for them to thrive under a system that is stacked against them, but it can’t stop there. This is why we aim to improve the lives of people with SCD by collaborating with communities to address the social determinants of health.
At Sanius Health, our wraparound model of care puts the needs of sickle cell disease (SCD) patients first, providing coordinated physical, mental, and social support. By taking a holistic view of health, we can reduce avoidable hospital admissions and enable timely discharges, freeing up capacity this winter.
By empowering members of our ecosystem to manage their condition, our approach aims to prevent complications, and avoid crisis situations that result in ED visits. Through partnerships across the NHS, our approach supports seamless transitions between primary, secondary, and community care. Our patient engagement team bridges gaps, while our insights enables collaboration between providers. This aligns care and helps meet demand, ahead of the pressures we can expect this winter.
In addressing the social determinants and inequities negatively impacting SCD outcomes, we can drive system-level change for future operational resilience this winter and beyond. To learn more, get in touch with the Sanius Health Team at: info@saniushealth.com
The patient experience shared.
Join the Sanius Health Community
Register your interest below and a member of our team will follow up with you soon.
