< Back to Sanius content
From Evidence to Everyday Insight: Connecting EHR, Wearables and Patient Voice to Transform Outcomes, Evidence and Care
A new model of care and evidence generation is emerging. One that connects what clinicians record, what patients report, and what real-time data shows.

By integrating EHR data, patient-reported outcomes and wearable signals, we are beginning to close the gap between clinical trials, real-world evidence and everyday patient experience.
NHS clinicians are now starting to receive structured patient updates ahead of appointments, giving early visibility into how patients have been feeling between visits. At the same time, patients are increasingly contributing to their own records, sharing blood results, private imaging such as MRI scans, and details from external appointments. For medical and HEOR teams, this represents a shift from fragmented datasets to a more continuous, patient-led evidence stream that better reflects real-world treatment experience and outcomes.
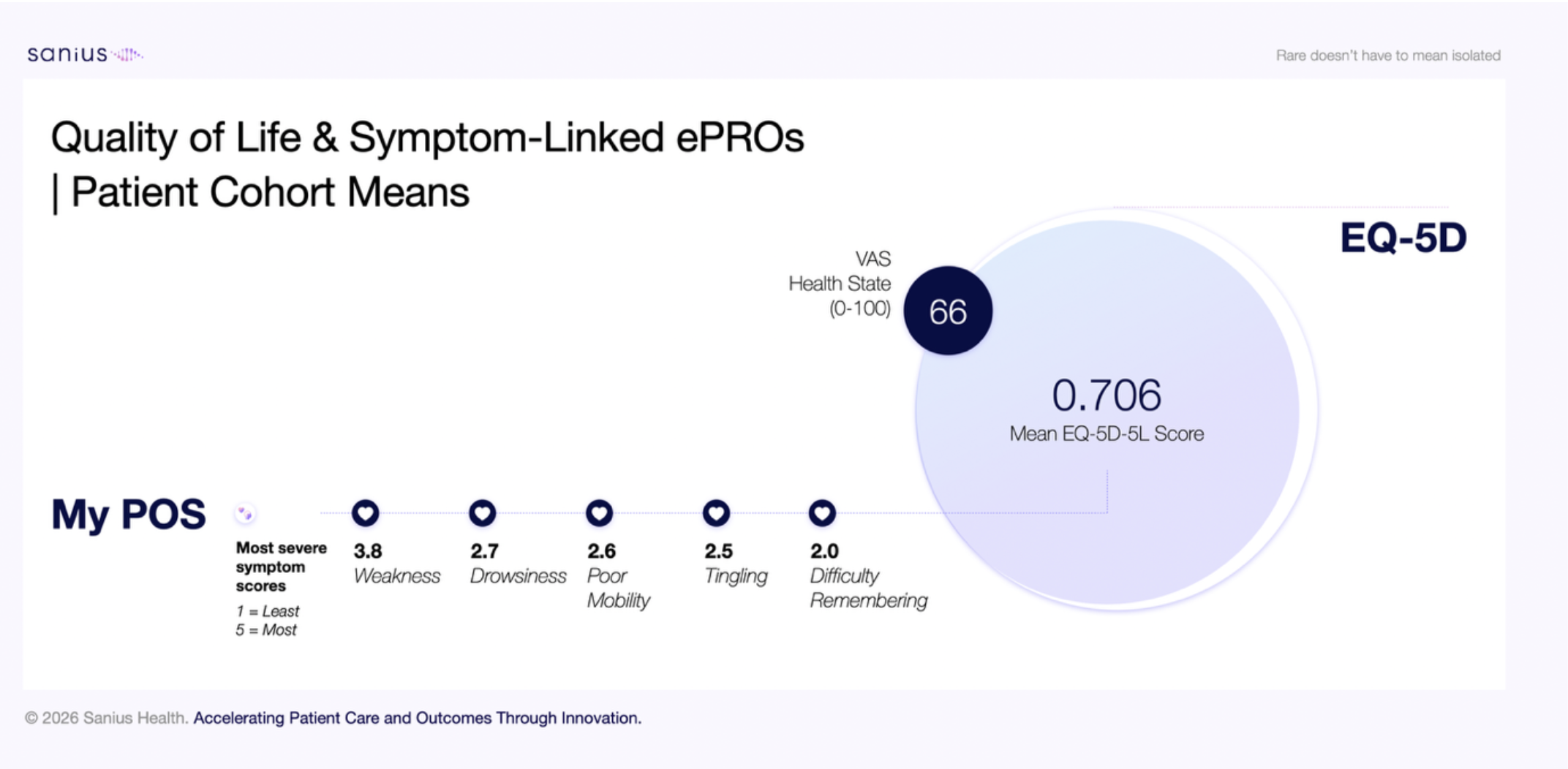
One of the most persistent challenges in healthcare and life sciences is understanding what happens between touchpoints. Clinical trials provide controlled insight. EHR systems provide longitudinal history. But neither fully captures the lived experience of patients on therapy. By combining EHR data with continuous patient-reported outcomes and wearable signals, we begin to close this gap. This creates a more complete evidence layer that supports not only clinical decision making, but also deeper understanding of treatment effectiveness, tolerability, and quality of life in real-world settings.
What the data now shows is both clinically meaningful and commercially relevant. In a cohort of Multiple Myeloma patients, thousands of real-world datapoints were captured across symptoms, activity, sleep, and clinical history. Patients consistently reported fatigue and drowsiness as the most severe symptoms, with severity scores approaching 4 out of 5. Higher daily activity levels were associated with lower symptom burden across multiple domains, including fatigue, appetite loss, and cognitive difficulty. Younger patients, often assumed to have better resilience, showed lower quality of life scores and higher psychological burden despite higher activity levels. When linked to EHR data such as treatment lines, medications, and co-morbidities, these findings provide a more nuanced view of treatment impact across patient subgroups.
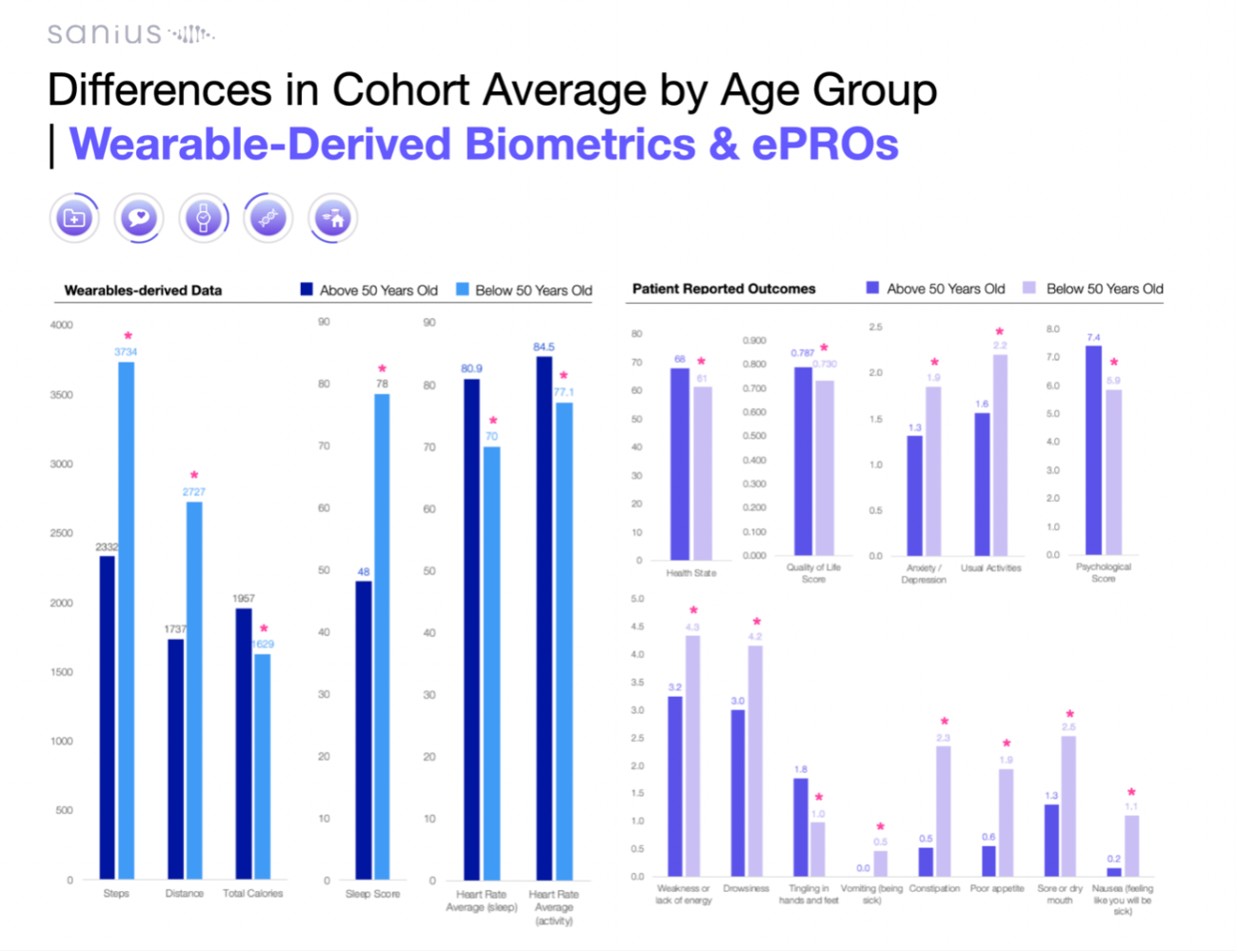
For medical and HEOR teams, this changes the nature of evidence. It enables earlier signal detection on treatment response and tolerability. It supports more granular patient stratification. It provides continuous quality of life and functional outcome data that can strengthen value dossiers, reimbursement discussions, and post-market evidence strategies. Importantly, it moves beyond static endpoints to dynamic, patient-centred measures that reflect how therapies perform in everyday life.
Integration is what unlocks this value. EHR data provides the clinical backbone. Wearables and patient-reported outcomes provide real-time resolution. Together, they create a longitudinal, high-frequency dataset that can support clinical care, regulatory conversations, and health economic modelling in parallel. This is not simply more data. It is a more complete and connected view of the patient journey.
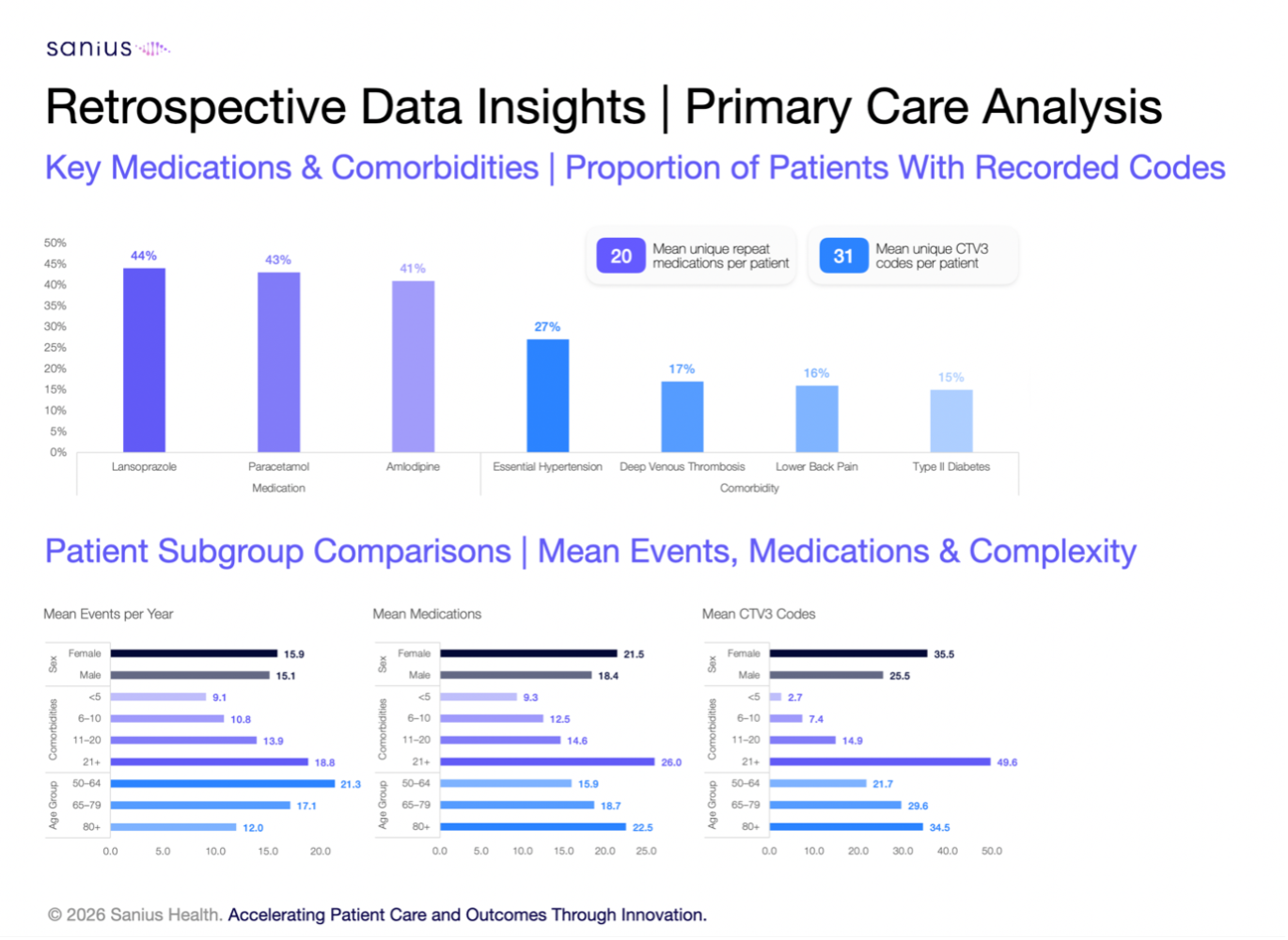
The impact is tangible. Earlier identification of deterioration supports timely intervention. Better understanding of treatment burden improves adherence and outcomes. Continuous insight into patient experience strengthens both clinical care and real-world evidence generation. Over time, this leads to more effective therapies, better patient outcomes, and more efficient healthcare systems.
The remaining challenge is not capability, but adoption. Embedding these data streams into clinical workflows and evidence frameworks in a way that supports clinicians, satisfies regulatory requirements, and delivers value to patients. The opportunity is clear. To bridge the gap between trials and reality, and to build an evidence model that reflects how patients actually live with disease.
For medical and HEOR leaders, the question is no longer whether this data exists. It is how it can be integrated, validated, and used to shape the next generation of clinical and commercial strategy.
The patient experience shared.
Join the Sanius Health Community
Register your interest below and a member of our team will follow up with you soon.
