< Back to Sanius content
BSH 2026: Shaping Research-Driven Care in Haematology Through New Haemophilia Baselines in Primary Care and Deep Patient Signals in SCD
As we head into BSH 2026, the shift is clear. Not away from science, but toward the patient signal. This is our fourth year contributing at the British Society for Haematology Annual Scientific Meeting, and the direction is sharper than ever.

The future of haematology will not be defined by isolated datasets or retrospective trials. It will be shaped by longitudinal, real-world evidence that reflects how patients actually live and deteriorate over time.
We have spent the last 2,000 days focused on one problem. How to generate meaningful evidence from longitudinal datasets that closes gaps in care delivery, addresses unmet patient need, and supports research colleagues and industry in accelerating new therapies. That work is now translating into clearer signals across both clinical and research settings.
Our work this year spans two areas. Haemophilia in primary care, and sickle cell disease through continuous monitoring. Different datasets, same problem. We are still missing critical context.
In haemophilia, primary care holds a longitudinal view of patients, but lacks structure where it matters. Severity is rarely captured in a usable form, limiting stratification and decision making.
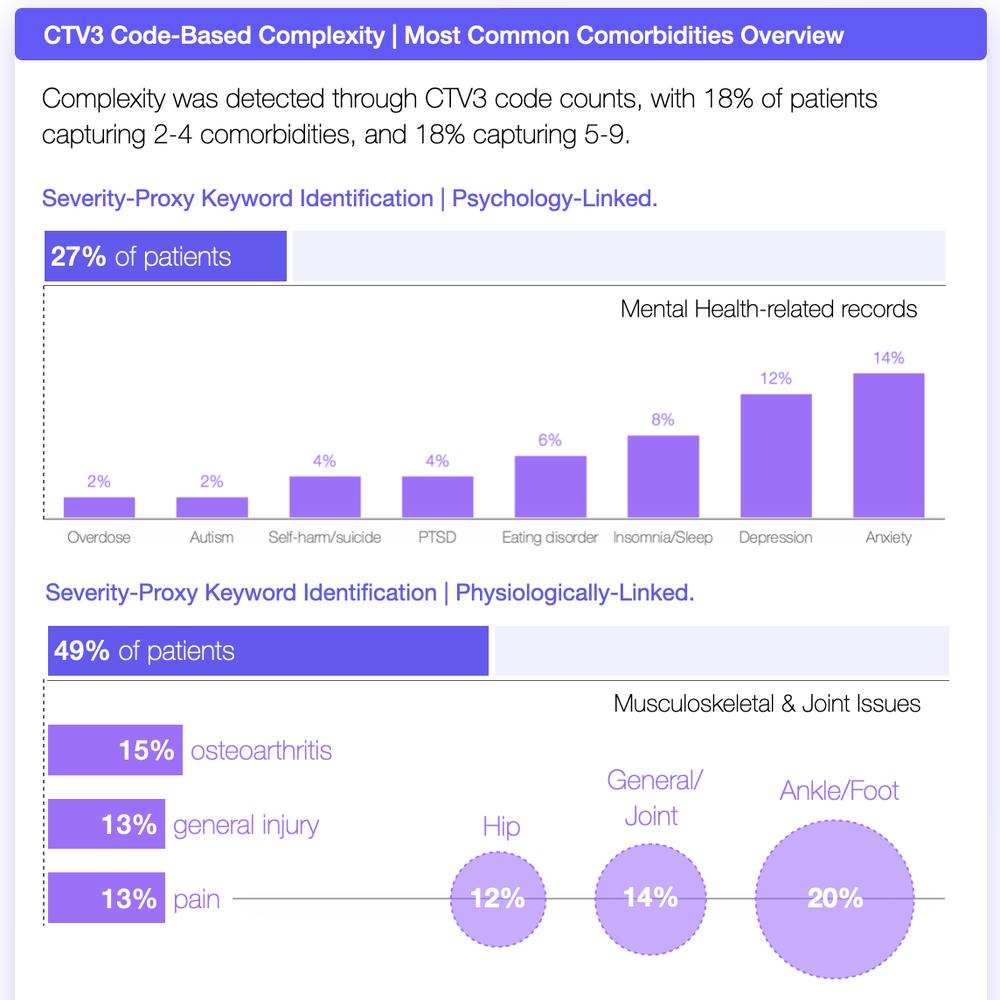
In our cohort, 18 percent of patients had two to four comorbidities, and another 18 percent had five to nine. Nearly half showed musculoskeletal or joint issues. Over a quarter had mental health records.
This is not noise. It is the disease burden playing out in real life.
Utilisation data reinforces the point. Eighty percent of patients had recorded appointments, with an average of six contacts per year. Primary care is where the majority of lived experience sits, yet it remains underpowered for research without severity and treatment context.
The opportunity is clear. Link it, enrich it, and it becomes one of the most powerful assets in haemophilia research.
Sickle cell disease shows what happens when we capture the right signals.
In a high burden cohort, we analysed repeated vaso-occlusive crises using wearable biometrics and patient reported outcomes. The insight is simple. Crises are not events, they are trajectories.
Activity metrics varied significantly across episodes, while PROs such as pain and quality of life remained more stable. Sleep and heart rate signals shifted meaningfully around crisis periods.
This creates a dual model. Wearables capture volatility. PROs provide stability.
Together, they move us toward personalised prediction. Not population averages, but patient specific insight into when a crisis is building and how it evolves.
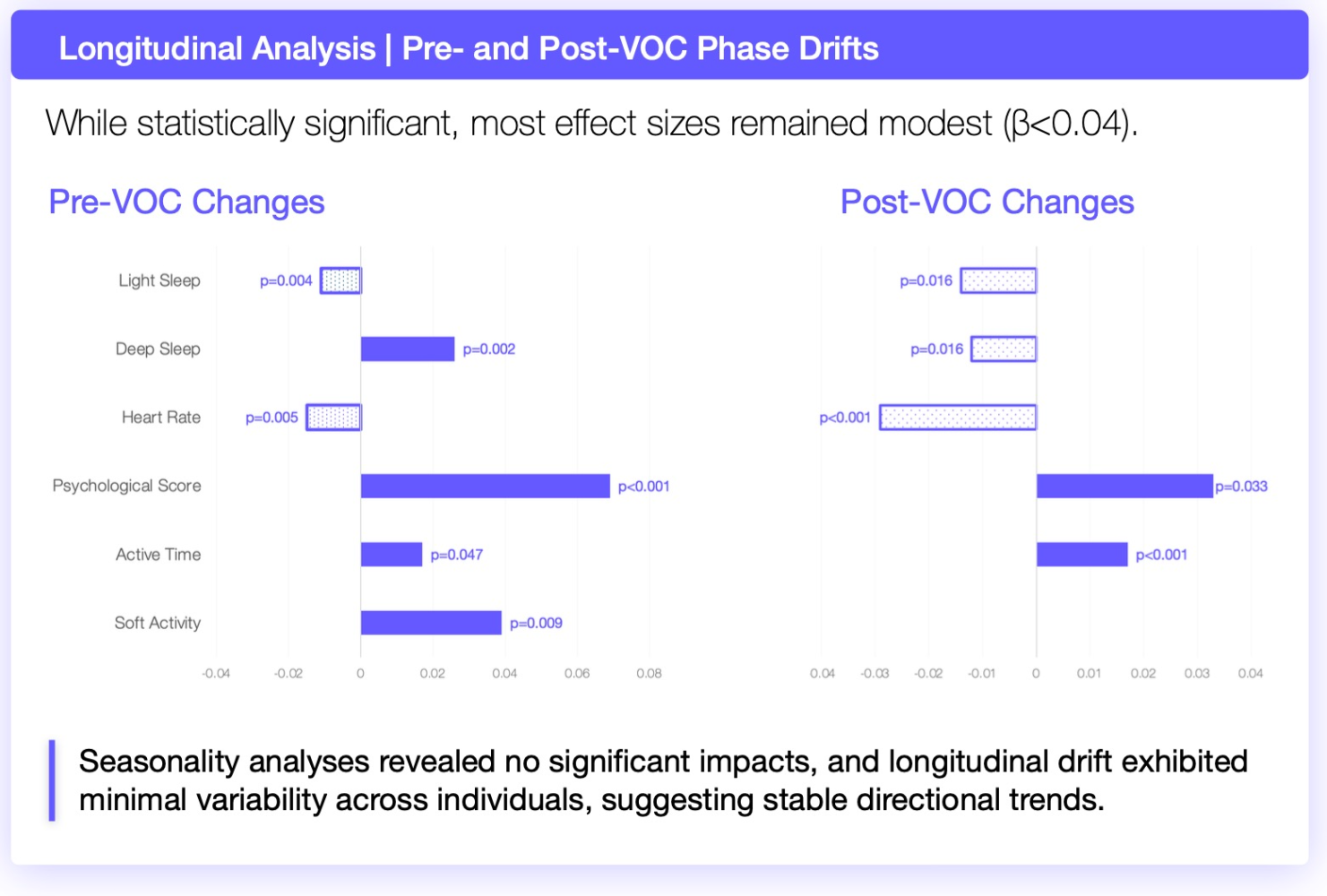
Across both studies, the pattern is consistent. The system captures fragments. Patients experience continuity.
The next phase is to close that gap:
· Link primary care with specialist datasets
· Embed severity and treatment pathways into routine capture
· Scale wearable and PRO driven models alongside traditional records
· Design around trajectories, not timepoints
This is not about adding complexity. It is about removing blind spots. And for patients, it means being properly represented in the data that drives their care.
We are looking forward to meeting colleagues at BSH 2026 in Liverpool. If you are attending and want to explore how primary care data, PROs and continuous monitoring can be combined to drive better research and outcomes in SCD and haemophilia, we would welcome the discussion.
Because the next step in haematology is not just better treatment.
It is better understanding.
The patient experience shared.
Join the Sanius Health Community
Register your interest below and a member of our team will follow up with you soon.
